8 Person centred care examples You Should Know

Person-centred care is more than just a buzzword; it's a practical approach that places you, your goals, and your preferences at the very core of your support services. It means moving beyond a one-size-fits-all model to a framework where your unique needs, values, and life circumstances guide every decision. This philosophy is fundamental to achieving meaningful outcomes in disability support, whether it's for in-home care, community access, or Supported Independent Living (SIL) in Adelaide and regional South Australia.
But what does this look like in the real world? How does a support worker or organisation translate these principles into tangible actions? This article provides clear, detailed person centred care examples to answer those questions. We will move past theory and dive into specific case studies that demonstrate this approach in action.
You will see precisely how strategies like shared decision-making, personalised care planning, and cultural responsiveness are implemented. Each example is broken down to reveal the specific tactics used, the strategic thinking behind them, and actionable takeaways you can apply or look for in your own support experience. Our goal is to equip you with a practical understanding of what high-quality, person-centred support truly entails, helping you make informed choices about your NDIS plan and providers.
1. Shared Decision Making
Shared decision-making is a cornerstone of person-centred care, transforming the traditional dynamic between a provider and an individual. Instead of a one-way flow of information, it establishes a collaborative partnership. In this model, both the support worker or healthcare professional and the individual bring essential expertise to the table. The provider offers clinical knowledge and options, while the individual contributes their personal values, life goals, and preferences.

This process ensures that any decision made truly reflects what is important to the person receiving support, aligning their care with their life, not the other way around. It's a fundamental shift from "What's the matter with you?" to "What matters to you?".
Strategic Breakdown
This approach is highly effective because it directly empowers the individual, fostering a greater sense of ownership and engagement in their own support plan. For NDIS participants, it’s about moving beyond being a passive recipient of services. Helping patients through accessible information is important for shared decision-making, exemplified by full patient guides explaining complex procedures like digital retinal photography. In disability support, this could mean co-designing a weekly schedule for community access or choosing between different assistive technologies.
Actionable Takeaways
- Implement Decision Aids: Use visual tools, checklists, or simple summaries to explain options, benefits, and potential drawbacks.
- Practise "Ask-Tell-Ask": First, ask what the person already knows or wants to know. Then, tell them the relevant information in clear, jargon-free language. Finally, ask them what they think about the information to check their understanding and gauge their reaction.
- Allocate Time for Questions: Ensure meetings are not rushed. Create a supportive environment where the individual feels comfortable asking questions and expressing concerns without feeling pressured.
- Follow-Up: After a decision is made, check in to see how it's working. Be prepared to adjust the plan based on their real-world experience.
This method is a powerful example of person-centred care in action, building trust and ensuring support is genuinely tailored to the individual's aspirations. To explore this concept further within the NDIS framework, you can learn more about supported decision making for NDIS participants.
2. Personalized Care Plans
Personalized care plans are a fundamental expression of person-centred care, moving beyond generic templates to create a truly individualised roadmap. These plans are co-developed with the individual, weaving together their specific medical history, lifestyle, preferences, and most importantly, their personal goals and social circumstances. This creates a full guide for coordinated support across multiple providers and settings.
This approach ensures the plan is a living document that reflects the person's real life, not just their diagnosis. For an NDIS participant, this means their support plan is built around their aspirations, whether that's learning a new skill, joining a community group, or increasing their independence at home. It’s a tangible commitment to putting the person first.
Strategic Breakdown
The power of a personalised care plan lies in its role as a central communication tool. It ensures that everyone involved, from support workers to allied health professionals and family members, is working from the same page and towards the same goals defined by the individual. Models like the NHS's personal health budgets and Geisinger's ProvenCare system demonstrate that this coordinated, goal-oriented approach leads to better outcomes.
The bar chart below visualises some of the significant impacts observed from implementing personalised care plans.
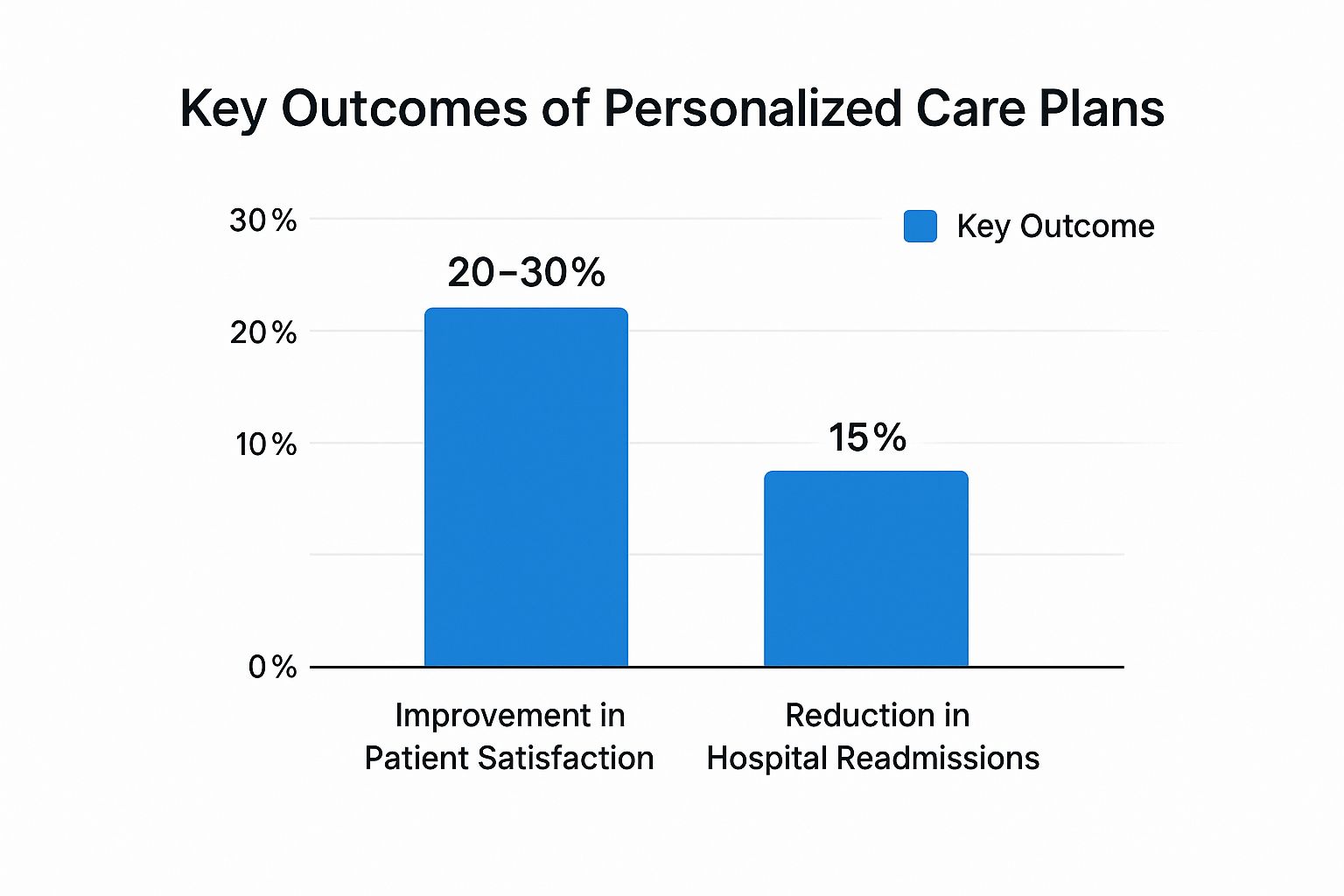
The data clearly indicates that when care is tailored to the individual, there is a notable rise in satisfaction and a measurable decrease in negative health events like hospital readmissions.
Actionable Takeaways
- Co-develop Goals: Involve the individual and their family or advocates in every step of developing the plan. Use their own words to describe their goals.
- Use Simple Language: Avoid clinical jargon. The plan should be clear, accessible, and easily understood by everyone, especially the person it is for.
- Schedule Regular Reviews: A person's needs and goals change. Schedule regular check-ins (e.g., quarterly) to review the plan and make updates as needed.
- Ensure Shared Access: Use a shared digital folder or a physical copy that is accessible to all members of the support team to ensure consistency in service delivery.
By truly personalising the planning process, support providers can deliver services that are not just effective but also meaningful. You can discover more about how personalised disability care transforms lives and brings personal goals within reach.
3. Patient Narratives and Storytelling
Using patient narratives and storytelling involves actively collecting and valuing an individual's personal story to better understand their world. This approach moves beyond clinical data and checklists, recognising that a person's life experiences, values, and perspective are important for shaping their support. By listening to their story, support providers gain deep insights that inform genuinely personalised care decisions.

This method honours the individual as the expert in their own life. It transforms the support relationship into one of mutual respect and understanding, where care plans are built not just on needs, but on identity, history, and personal meaning. This is a profound example of person centred care because it places the person's unique voice at the core of all activities.
Strategic Breakdown
This strategy is effective because it builds empathy and connection, providing context that is often missed in formal assessments. For an NDIS participant, their narrative might reveal a past passion for gardening or a specific fear about community transport, details that are essential for designing meaningful and successful support. Initiatives like The Schwartz Center for Compassionate Healthcare use storytelling rounds to help staff connect with the emotional side of care, leading to reduced burnout and more compassionate service delivery.
Actionable Takeaways
- Create Safe Spaces: Dedicate specific, unhurried time for conversations that aren't focused on a checklist. This could be during a relaxed home visit or a planned review meeting.
- Train in Active Listening: Equip support workers with skills to listen without interrupting, ask open-ended questions that encourage storytelling, and reflect back what they hear to confirm their understanding.
- Use Narrative Prompts: Start conversations with gentle prompts like, "Tell me about a time you felt really included in your community," or "What does a really good day look like for you?".
- Protect Privacy: Always ensure you have clear consent to record or share any part of a person's story and be transparent about how it will be used to improve their support.
4. Patient Advocacy Programs
Patient advocacy programs formalise the support an individual receives when working through complex support or healthcare systems. These structured programs provide a dedicated advocate who acts as a guide, translator, and champion for the person, ensuring their voice is not just heard but is central to all decision-making. This is a powerful example of person-centred care as it provides an essential bridge between the individual and the often-intimidating environment of healthcare or disability services.
The advocate’s role is to help the person by demystifying processes, explaining rights, clarifying options, and communicating the individual’s wishes to providers. This ensures that the care plan is built around the person’s unique needs and goals, rather than forcing them to fit into a pre-existing service model. For an NDIS participant, this could mean having an advocate help them prepare for a plan review meeting or resolve a conflict with a service provider.
Strategic Breakdown
This approach is highly effective because it addresses the inherent power imbalance that can exist between individuals and large institutions. By providing a knowledgeable and dedicated ally, advocacy programs level the playing field, making the system more accessible and responsive. It reinforces the principle that support services should work for the individual, not the other way around. This fosters confidence and self-advocacy skills over time.
For instance, an advocate might help a person with a communication disability articulate their preferences for their daily routine in a Supported Independent Living (SIL) environment, ensuring support workers understand and respect their choices. This direct support helps turn the goals of an NDIS plan into tangible, everyday realities.
Actionable Takeaways
- Establish Clear Roles: Define the advocate's responsibilities and boundaries from the outset. Ensure everyone, including the individual and their support team, understands the advocate is there to support the person's voice, not to make decisions for them.
- Provide Full Training: Advocates must be skilled in communication and have a deep understanding of the relevant systems, like the NDIS. Training should cover everything from working through the NDIS portal to effective negotiation techniques.
- Integrate Advocates into Teams: Encourage advocates to be part of care team meetings and planning sessions. This collaborative approach ensures the person’s perspective is embedded in the support strategy from the beginning.
- Create Feedback Loops: Regularly seek feedback from the individual about the advocacy process. This helps refine the program and ensures it remains genuinely centred on their needs and experiences.
Effective advocacy is a cornerstone of a system that truly values individual autonomy and choice. To see how this principle extends into broader community settings, you can explore the role of community support in disability support.
5. Cultural Competency and Culturally Responsive Care
True person-centred care extends beyond individual preferences to embrace and respect a person’s entire cultural identity. Culturally responsive care involves recognising and integrating an individual's cultural, linguistic, and social background into their support plan. It moves away from a one-size-fits-all model to deliver services that are meaningful and appropriate within the context of a person’s beliefs, traditions, and values.
This approach is important in a diverse society, ensuring that support is not only effective but also respectful and validating. For NDIS participants from culturally and linguistically diverse (CALD) backgrounds, this means their support workers understand specific communication styles, family structures, dietary needs, or religious practices that are central to their wellbeing. It acknowledges that culture profoundly shapes a person’s view of health, disability, and support.
Strategic Breakdown
This model is a powerful example of person-centred care because it addresses the whole person, preventing cultural misunderstandings that can create barriers to effective support. By actively seeking to understand a person's cultural context, providers can build deeper trust and rapport. For instance, in disability support, this might involve scheduling services around important religious observances, engaging with family members in a culturally appropriate manner, or sourcing food for meal preparation that aligns with cultural norms. This demonstrates a commitment to seeing the individual beyond their diagnosis.
Actionable Takeaways
- Conduct Cultural Assessments: As part of the initial intake process, gently ask questions about cultural background, communication preferences, and any specific traditions or values that are important to the individual and their family.
- Hire a Diverse Team: Actively recruit support workers from various cultural backgrounds. Having staff who speak different languages and understand diverse customs is invaluable.
- Provide Ongoing Training: Implement regular cultural competency training for all staff to raise awareness and equip them with the skills to provide respectful, non-judgemental care.
- Use Professional Interpreters: When a language barrier exists, use professional interpreting services rather than relying on family members to ensure information is conveyed accurately and confidentially.
Integrating these practices ensures that care is not just personalised but also culturally safe and inclusive. To better understand its application, you can explore cultural competency in disability support.
6. Comfort and Dignity Preservation
Preserving comfort and dignity is a fundamental aspect of person-centred care, ensuring that an individual’s sense of self and respect is maintained throughout their support experience. This approach moves beyond clinical tasks to prioritise the human experience, making sure people feel valued, safe, and heard. It acknowledges that true care addresses not just physical needs but also emotional, spiritual, and personal well-being.
This principle is about recognising the inherent worth of every individual, regardless of their support requirements. In a disability support context, it means creating an environment where a person's privacy is protected, their choices are honoured, and they are treated as an equal partner in their care. It is one of the most important person centred care examples because it forms the bedrock of trust between an individual and their support worker.
Strategic Breakdown
This approach is highly effective because it directly addresses the potential for vulnerability that can come with receiving support. By actively preserving dignity, support workers build profound trust and psychological safety, which encourages open communication and greater participation from the individual. For NDIS participants, this might mean a support worker ensuring personal care routines are handled discreetly and according to the person's specific preferences, or creating private spaces for sensitive conversations about their support plan. Organisations like the Picker Institute have long championed these values, emphasising that care must be respectful and tailored to individual needs and values.
Actionable Takeaways
- Practise Dignity-Preserving Communication: Train support workers to always knock before entering a room, ask for permission before providing physical assistance, and use respectful, non-patronising language.
- Establish Clear Privacy Protocols: During the planning phase, explicitly ask about and document preferences regarding personal space, modesty, and the sharing of information. For instance, "How would you like me to assist you in the bathroom to ensure you feel comfortable and respected?"
- Prioritise Comfort in the Environment: Simple adjustments like ensuring a room is at a comfortable temperature, offering a preferred blanket, or playing their favourite music can make a significant difference to a person's sense of well-being.
- Respect Personal Routines: Learn and adhere to an individual's established daily routines and preferences, from how they like their coffee to the time they prefer to wake up. This validates their autonomy and sense of control.
7. Family and Caregiver Integration
Family and caregiver integration is a full approach that moves beyond treating an individual in isolation. It recognises that family, friends, and other informal carers are often central to a person's life and wellbeing, viewing them as essential partners in the care experience. This model involves them in care planning, decision-making, and daily support, ensuring a cohesive and unified approach.
This method actively listens to and values the unique insights that family members provide, as they often know the individual's history, preferences, and subtle communication cues better than anyone. It’s about creating a circle of support where everyone, including the participant, support workers, and family, is aligned and working towards the same goals. This whole-person view is a powerful example of person-centred care in practice.
Strategic Breakdown
Integrating families is highly effective because it builds a stronger, more resilient support network. This reduces the risk of miscommunication and ensures consistency in care, especially in environments like Supported Independent Living (SIL) where multiple people are involved. For an NDIS participant, this could mean having a family member help communicate their goals during a planning meeting or providing input on a behaviour support plan. It acknowledges the family's role and provides them with the resources and respect they need to participate effectively.
Actionable Takeaways
- Establish Clear Communication Channels: Use a shared communication book, a dedicated group chat, or regular family meetings to keep everyone informed about progress, challenges, and upcoming appointments.
- Provide Education and Training: Offer family members training on specific equipment, communication techniques, or aspects of the person's disability. This empowers them to provide confident and competent support.
- Develop Family Advisory Councils: In larger organisations, creating a formal council for family members to provide feedback on services and policies can embed their perspective into the core of operations.
- Respect Family Dynamics: Acknowledge and respect the unique culture, values, and dynamics of each family. Always ensure the person receiving support is at the centre of decisions about who is involved and how.
8. Continuous Feedback and Quality Improvement
A commitment to continuous feedback and quality improvement is a powerful demonstration of person-centred care. This approach establishes systematic processes for actively seeking, analysing, and acting upon feedback from individuals receiving support. It transforms the relationship from a static service delivery model to an evolving partnership, where the individual’s voice directly shapes the quality and direction of their care.
This ongoing dialogue ensures that services do not just meet a baseline standard but are consistently refined to better align with the person's changing needs, preferences, and satisfaction. It's about creating a culture where feedback isn't seen as a complaint but as a valuable tool for growth and excellence.
Strategic Breakdown
This strategy is effective because it makes an organisation accountable to the people it supports. For NDIS participants, it provides a structured and safe way to share their experiences, good or bad, knowing that their input will lead to tangible improvements. This process builds trust and reinforces that their perspective is valued. Instead of a one-off satisfaction survey, this is about embedding a responsive loop into every aspect of service delivery, from the compatibility of a support worker to the effectiveness of a community access program.
Actionable Takeaways
- Use Multiple Feedback Channels: Offer various ways for individuals to share their thoughts, such as simple text-message surveys, one-on-one check-ins with a trusted coordinator, or anonymous online forms.
- "Close the Loop": Always communicate back to individuals about the feedback received and the changes being implemented. This shows their input has been heard and acted upon.
- Train Staff in Receiving Feedback: Equip your team with the skills to receive feedback constructively and without becoming defensive, turning every interaction into an opportunity for improvement.
- Focus on Actionable Insights: Analyse feedback to identify recurring themes and prioritise changes that will have the most significant positive impact on the individual's experience.
By embedding these practices, support providers can ensure their services remain dynamic and genuinely person-centred. To discover how to integrate these systems effectively, you can learn more about continuous feedback and quality improvement strategies.
8 Key Person-Centred Care Examples Comparison
| Approach | 🔄 Implementation Complexity | 💡 Resource Requirements | 📊 Expected Outcomes | 💡 Ideal Use Cases | ⭐ Key Advantages |
|---|---|---|---|---|---|
| Shared Decision Making | Moderate to high due to need for training and time-intensive consultations | Requires trained providers and decision aids | Improved satisfaction, adherence, reduced decisional conflict | Patient-centered care where values impact decisions | Enhanced patient engagement and trust |
| Personalized Care Plans | High complexity due to coordination across multiple providers | Resource-intensive, needs system integration and regular updates | 20-30% satisfaction improvement, 15% readmission reduction | Complex conditions requiring coordinated care | Targeted interventions and efficient resource use |
| Patient Narratives and Storytelling | Moderate, involves structured collection and analysis | Time-intensive, requires privacy safeguards | Improved empathy, patient validation, reduced provider burnout | Improving provider understanding and empathy | Deep insights into patient experience |
| Patient Advocacy Programs | Moderate to high, staffing and training of advocates necessary | Additional personnel and training costs | 20% reduced hospital stays, 25% better treatment completion | Navigation support for complex healthcare systems | Better coordination and reduced disparities |
| Cultural Competency and Responsive Care | Moderate, requires ongoing training and organizational change | Continuous training, diverse staff, community engagement | Improved outcomes and reduced disparities | Diverse populations needing culturally appropriate care | Enhanced communication and patient trust |
| Comfort and Dignity Preservation | Low to moderate, depends on staff training and environment design | Facility investment, staff training | Improved patient experience, reduced anxiety | Settings prioritizing patient comfort and autonomy | Promotes respect, privacy, and healing environment |
| Family and Caregiver Integration | Moderate, coordination and training needed | Resources for education, support groups, respite services | 15% reduced hospital stays, 25% improved satisfaction | Care involving family in planning and delivery | Strengthens care continuity and reduces caregiver stress |
| Continuous Feedback & Quality Improvement | Moderate to high, requires data systems and analysis capability | Resource-intensive data collection and management | Continuous quality improvement, enhanced satisfaction | Organizations targeting ongoing enhancement | Data-driven improvements and patient loyalty |
Final Thoughts
Throughout this article, we've journeyed through a series of detailed person centred care examples, moving beyond abstract theory to showcase what this approach looks like in the real world. From co-designing care plans that honour an individual's unique goals to integrating family members as true partners in the support experience, the core message is clear: authentic person-centred care is an active, ongoing collaboration. It’s not a checklist to be completed, but a dynamic philosophy that must be lived out in every interaction.
The examples we've explored, covering everything from shared decision making and culturally responsive practices to preserving dignity in daily routines, all share a common thread. They demonstrate a fundamental shift in the power dynamic, placing the individual with a disability firmly in the driver's seat of their own life and support services. This is about recognising that the person is the foremost expert on their own needs, preferences, and aspirations.
Key Principles for Your Practice
As you reflect on these examples, remember the most powerful takeaways are not just the outcomes, but the processes that led to them.
- Active Listening is Non-Negotiable: The foundation of all person-centred practice is listening to understand, not just to respond. It's about hearing what is said and, just as importantly, what is left unsaid.
- Flexibility Overcomes Rigidity: Pre-made templates and one-size-fits-all solutions are the enemies of personalised care. The best support plans are adaptable, ready to evolve as a person's life, goals, and circumstances change.
- Small Gestures Create Big Impact: As seen in our examples, preserving dignity and showing respect often comes down to small, consistent actions. Asking for preference, explaining a process, or simply taking an extra moment to connect can make all the difference.
Putting Person-Centred Care into Action
Mastering these concepts is more than just good practice; it is essential for fostering genuine independence, wellbeing, and fulfilment. When support is truly centred on the person, it empowers them to build skills, engage with their community in meaningful ways, and live a life that reflects their own values. This approach transforms support from a service being delivered to someone into a partnership built with them.
Ultimately, the goal is to move beyond simply providing services and towards creating environments where people can thrive on their own terms. The person centred care examples in this guide are not just success stories; they are a strategic roadmap. They offer a blueprint for building trust, fostering autonomy, and delivering support that is as unique as the individual receiving it. This is the future of disability support in Adelaide, regional South Australia, and beyond - a future built on respect, partnership, and choice.
Ready to experience what truly personalised support feels like? At Vana Care, our entire model is built on the principles discussed in these person centred care examples, ensuring you are always at the centre of every decision. Visit Vana Care to discover how our dedicated team can partner with you to achieve your goals.
Thinking about Supported Independent Living in Adelaide? Our team can walk you through your options.



Stay up to date
Follow Our Story
See what our team and participants get up to around Adelaide. Real stories, community events, and a look behind the scenes at how we do disability support differently.